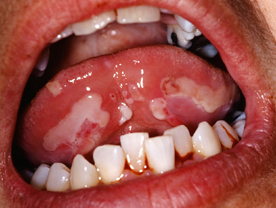
Pemphigus Vulgaris : It is the most common variant. The disease commonly starts as superficial large irregular ulcers in the mouth. The ulcers do not heal for prolonged periods and keep recurring. After a variable period of a few months to several years, the skin also starts developing vesicles and bullae which are characteristically flaccid and present on apparently normal-looking skin. The bullae change into superficial large ulcers which often extend peripherally and do not heal for prolonged periods. Crusting and secondary infection are common. The skin lesions may appear on any part of the body, and often involve large areas. Involvement of the mucosal areas may include one or more of the oral mucosa, the nasal mucosa, pharynx, larynx, conjunctiva and genital and the anal areas. Recurrences are frequent The disease is associated with a very high degree of morbidity and mortality, even though other systemic organs are not involved.
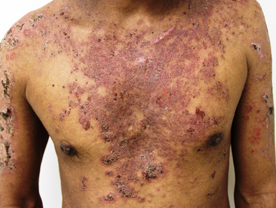
Pemphigus Foliaceous : It is the second variant but it is much less common compared to pemphigus vulgaris. It manifests chiefly with scale-like lesions which are actually the tops of the superficial blisters. A few well formed blisters may also be seen. The mucous membranes are generally not involved in this variant but involvement of the skin may he so extensive as to resemble exfoliative dermatitis. The patient with this disease has better life expectancy.
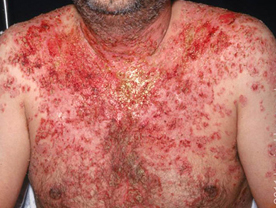
Pemphigus Erythematosus : This is the third variant and resembles pemphigus foliaceous but the lesions tend to form crusts on the cheeks, scalp and the upper chest to resemble lupus erythematosus and most of the lesions tend to have redness around the skin lesions. Such patients however do not have any other clinical manifestations of SLE.
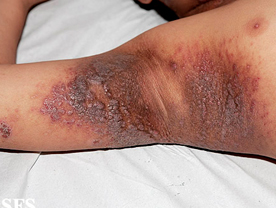
Pemphigus Vegetans :This is the least common variant and manifests as vegetating lesions in the folds of the skin especially the groins, axillae and the genitalia. The vegetations are formed by the proliferation of the base of the ulcers.
Diagnosis : The diagnosis in these cases can be confirmed by demonstrating acantholytic cells (Tzanck cells) in the smears made from the base of the blisters
ulcers and stained with Giemsa or Leishman stain (Tzanck Smear). Histopathological study of a fresh blister taken by biopsy would reveal an intra-epidermal acantholytic split which is suprabasal in pemphigus vulgaris and pemphigus vegetans, and subcorneal in pemphigus foliaceous and
pemphigus erythematosus. A direct immunofluorescence on the skin biopsy would reveal deposition of antibodies in an intercellular pattern while the patient
blood would contain similar antibodies which can react with the intercellular substance of the normal epidermal or epithelial tissue.
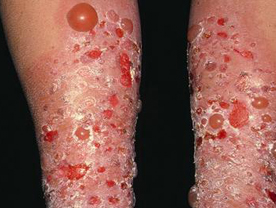
Pemphigoid : This is another auto-immune disease in which the IgG antibodies are directed against some component of the basement membrane. The blisters are therefore formed at the dermo-epidermal junction and are sub-epidermal Clinically, the blisters are large and tense and may be associated with crythema in the surrounding skin. Involve-ment of the mucous membranes is less common. The disease is not as fatal as pemphigus, but recurrences are common.
Diagnosis : The diagnosis can be established by taking a skin biopsy which would reveal a dermo-epidermal split A direct immunofluorescence test would demonstrate
deposition of IgG antibodies at the basement membrane zone and an indirect immunofluorescence test would reveal the presence of circulating IgG antibodies in the blood directed against the basement membrane zone.
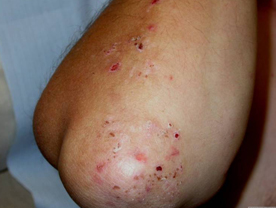
Dermatitis Herpetiformis : This s another vesiculo -bullous disorder which is based unity In this disease, there is deposition of at the tips of the dermal papillae. Clinically The disease is characterised by recurrent episodes of intense itching and eruptions of grouped papules, papules-vesicle or vesicles on the skin over the trunk and extremities. This
Disease in addition is associated with an enteropathy which may he completely asymptomatic in some patients. It can however sull be demonstrated by endoscopic examination of the small intestine which would reveal atrophic villi. The disease is common at two different age periods and is known as the juvenile form when it occurs in children between 5 to 10 years in age, and the adult form when it occurs in the adults.
Diagnosis : The splits in this disease also are dermoepidermal but active lesions reveal accumulation of polymorphs at the tips of the dermal papillae. A direct Immunofluorescence staining test on skin reveals deposition of lgA anibodies in clumps a the tips of the dermal papillae.
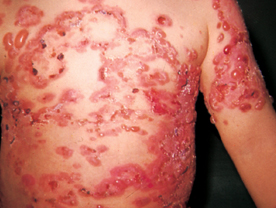
Benign Bullous Dermatosis of Childhood : This disease occurs in children and manifests as recurrent eruptions of tense bullae appearing on any part of the body In some cases there may also be erythema around the skin lesions. Mucous membranes are not involved. The disease disappears as the child grows up, but there are usually several recurrences during childhood. A similar linear lgA dermatosis is also occasionally seen in the adults and is known as the linear lgA disease.
Diagnosis : The blisters in these cases are sub epidermal and there is deposition of lgA anibodies in linear fashion at the dermo-epidermal junction.
Lupus Erythematosus : This disease belongs to another category of auto-immune diseases where a multitude of antibodies are directed against a variety of tissue components. Thus the manifestations of this disease can be present in several organs of the body.
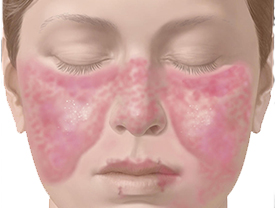
Systemic Lupus Erythematosus (SLE):In SL.E, there is a variety of antibodies directed against several tissue components, the major antibody being antinuclear antibody directed against the double stranded DNA. The clinical manifestations include fever, arthritis arthralgia, lymphadenopathy, weight loss and loss of appetite in almost all the cases. In addition, hepato-splenomegaly, polyserositis, glomerulonephritis, epilepsy, peripheral neuropathy, mental disturbances, myocarditis. amenorrhoca and Raynaud's phenomenon are present in a variable number of patients. The skin lesions consist of diffuse erythema and oedema, on the cheeks and the bridge of the nose. Less commonly, the lesions may be located on other parts of the face and other sun-exposed areas of the skin. There is no itching or pain, and the lesion is no ender Sometimes, SLE may manifest in the form of Urticaria, urticarial vasculitis, purpura, vesiculo-bullous lesions, non descript maculo papular eruptions. Lividoreticularis, telangiectasia on the posterior nail-folds finger-tip ulcers, superficial gangrene of the fingers and toes diffuse hair loss from the scalp, patchy cicatricial alopecia Ulcerations on buccal mucosa and crusted lesions on the lips.
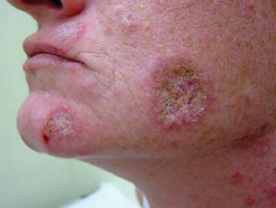
Discold Lupus Erythematosus (DLE):In some patients the disease is restricted to the skin and manifests with well-defined erythematous and scaly plaques with atrophy and depigmentation in the centre and well-defined hyperpigmented border The scales have characteristic projections on their under surface which correspond to the dilated openings of the cutaneous appendages (keratotic plugs), and are visible only on removing the scales (carpet tacks sign) There are no systemic manifestations. Such lesions are usually few and localized to the cheeks and the bridge of the nose(butterfly area). Occasionally here are several such lesions which are then present on the other sun-exposed pants of the body and sometimes oven on the unexposed parts Such patients are designated to have disseminaed discoid lupus erythematosus.
Diagnosis :
The diagnosis in lupus erythematosus is made on the basis of. (1) clinical manifestations of the disease, (2) characteristic histopathological changes in the skin biopsy taken from the lesion. (3) demonstration of deposition of the antibody in the basement membrane zone in the lesional skin and also in the clinically un-involved skin in cases having SLE, and (4) detection of the antinuclear antibodies in the blood of the patient in SLE In addition, thorough investigations are necessary in each case to determine the extent of involvement of the other organ systems.
Scleroderma : This is another auto-immune disoder in which multiple antibodies acting against a variety of antigens in the body produce diverse clinic manifestation.
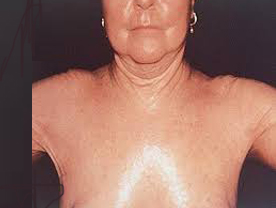
Systemic Sclerosis : The generalized form of the disease is called systemic Sclerosis or progressive systemic sclerosis PSS). It is a slowly progressive disease which commonly starts with Raynaud's phenomenon manifesting as pallor of the hand and feet on exposure to cold followed by bluing and then redness and swelling. Subsequently, the patient starts developing thickening and darkening of the skin which gets bound down to the underlying structures and cannot be lifted-up to make a fold. The epidermis becomes atrophic and shiny. These changes usually start from the fingers the toes and the face leading to thin tapering fingers (sclerodactyly), resorption of the terminal phalanges and nails, thin lips, atrophic nose and loss of naso-labial folds The skin changes progressively spread proximally to involve the entire body. Some patients also develop punctate depigmentation on the upper chest, upper arms and other areas. The systemic involvement consists of difficulty in swallowing, epigastric pain caused by oesophagitis, dyspnoea on exertion, arthralgia/arthritis amenorrhoea, renal involvement and occasionally fever.
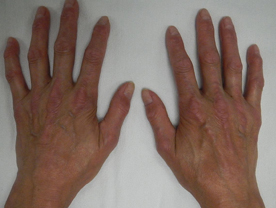
Crest Syndrome : Some patients have only calcinosis, Raynaud's phenomenon, oesophagial dismotility, sclerodactyly and telangiectasia which is called Crest syndrome.
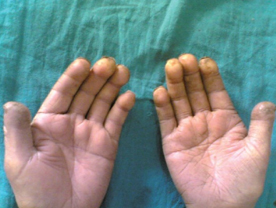
Acrosclerosis : Association of Raynaud's phenomenon with thin tapering fingers and sclerosis of the skin on the fingers and hands is called acrosclerosis.
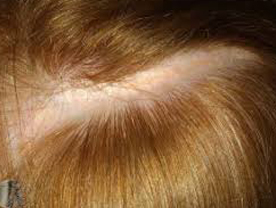
Morphoea : This term is used when a patient has a circumscribed area of indurated skin with hyperpigmentation. The skin in this area is atrophic and shiny. Such an area may be present on any part of the body. With time, the oedematous swelling disappears leaving behind a depressed and atrophic area. Localization of such an area on hairy skin leads to cicatricial alopecia. If the lesion is linear in shape it is called linear morphoea. Occasionally, a patient may have multiple lesions of morphoea scattered on different parts of the body. This is called generalized morphoea. Guttate morphoca is the term used when there are small punctate spots of white thickened skin.
Diagnosis :The diagnosis of morphoea or systemic sclerosis can be confirmed by a skin biopsy. Patients
having systemic sclerosis in addition have a variety of auto-antibodies in their blood, of which Scl-70 is the most specific but not present in all the cases. Other investigations are needed to determine the extent of involvement of other organs of the body.

