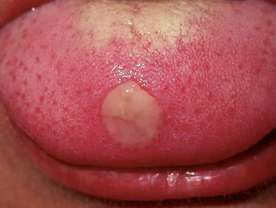
Primary Syphilis : The incubation period is 9-90 days although in most of the ases the irst manifestation appears between 2-4 weeks alter the iofection. The first lesion is a painless ulcer chancre) which is indurated, well-defined and located in the genital area The regional lymph nodes are also onlarged. non-tender, fim and discrete in the female, the ulcer may be located on the yaginal wall or the cervix uteri and thus may not be visible. The ulcer tends to heal even without any treatment. The diagnosis can be confirmed by demonstrating the Treponema pallidum by dark ground microscopy in the serous exudate obtained from the ulcer The serological test for syphilis (VDRL test) also becomes positive within 1-2 weeks after the appearance of the ulcer.
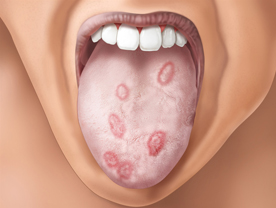
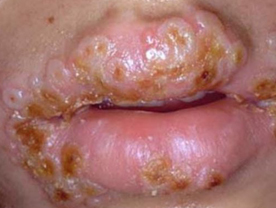
Secondary Syphilis : If the disease is not treated, 6-8 weeks after the appearance of the primary chancre the patient starts developing the signs and symptoms of secondary syphilis. The gener symptoms during this phase include headache, malaise anorexia, loss of weight, low grade fever, and pain in the muscles, bones and joints. The cutaneous lesions consist of generalized eruptions of completely asymptomatic and bilaterally symmetrical erythematous macules, papules and papulo-squamous or pustular lesions. Vesicles are never seen in this stage of syphilis. Papular lesions are the most common and when present in moist areas such as aroun the anus, intergluteal fold, vulva, groins and other skin folds they tend to become large fleshy masses and are called condyloma lata. Superficial linear or zigzag ulcers on the mucous membranes of the mouth or the genitals (snail tract ulcers), erythematous pigmented scaly lesions on the palms and soles, patchy loss of hair from the scalp
and generalized enlargement of the lymph nodes which are discrete, non-tender and rubbery in consistency are the other characteristics of the secondary syphilis. Some patients may also develop uveitis, arthritis, hepatitis or meningitis
The diagnosis of secondary syphilis is confirmed by demonstrating the Treponema pallidum from the skin and the mucosal lesions especially the condyloma lata. The VDRL test on blood is always positive although sometimes the test may show false negativity because of the very high titre. The lesions tend to heal even without any treatment but recurrences are common and this may continue for as long as 2 years. Ultimately however, the disease becomes clinically quiescent in all cases.
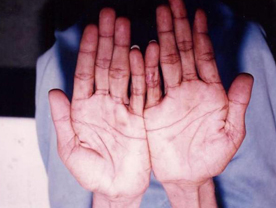
Latent Syphilis : The period after the secondary syphilis during which there is no clinical evidence of syphilis but the VDRL test on blood is positive while the cerehrospinal fluid is negative, scalled latent syphilis. The duration of latent syphilis is variable and may last a few years or the rest of the patient's Life.
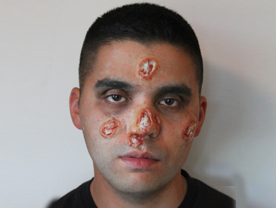
Tertiary Syphilis : Teiary sophilis can develop any time 3-10 years after the primary infection The earliest manifestations of tertiary ophilis include gummatous lesions which may involve the skinmucous membranes.subcutancous, submucosal issue, bonc, joints, muscles, heart, kidneys, brain, in fact any tissuc of the body. A gumma starts as a nodule which dull red in colour when present on the skin or produces symptoms of space occupying lesions when present in the organs. They can also lead to fracture when present the bone or produce characteristic punched out ulcers when present on the skin or mucous membrane. On healing, the gummas leave behind tissue paper scars. The diagnosis can be confirmed by a biopsy which shows a classical granuloma on histopathology
The other manifestations of tertiary syphilis include ular syphilis and neurosyphilis which by and are hardly ever seen these days because of proper ment during the carly phases of syphilis which pents the later stages of syphilis. Even gumma are enety uncommon.
The serological test for syphilis (VDRL. test) is usually posve at this stage but it may be negative The infectivity of syphilis is fairly high during the promary and the secondary stages of syphilis when the lesions and the secretions are teaming with the spirochactes while in the later part of the latent phase during the tertiary phase the infectivity is almost nil. On n average a patient is non-infectious after 2 ollowing the primary infection.
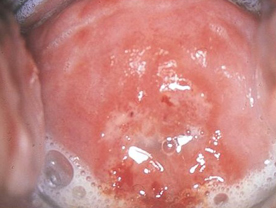
Gonorrhoea : It is caused by Neisseria gonorrhoeae which is a Gram negative diplococcus. The incubation period varies between 24 hours to 10 days. The earliest symptoms in the males can be a burning sensation in the urethra especially when passing urine and frequency of micturition and a discharge of thick yellowish pus from the urethra. In the female the infection usually occurs in the cervix uteri with purulent discharge. The vagina is generally not involved except in the prepubertal girls. Infection in the urethra and or the rectal mucosa may also occur but is relatively less frequent in the females.
The infection may be totally asymptomatic in both the sexes but especially in the females. If untreated the infection in males can ascend to involve the prostate, the seminal vesicles and the epididymis and produce signs and symptoms pertaining to the respective glands. Some patients may also develop arthritis, hepatitis, skin rashes septicaemia, endocarditis, myocarditis. pericarditis and even meningitis.
This infection can also spread to the paraurethral and the other glands along the urethra.
The diagnosis can be confirmed by preparing a smear from the pus discharge/secretion, staining it with Gram's stain and looking for Gram negative intracellular diplococci. It can be further confirmed by culturing the organisms on enriched media/selective media and identifying the organisms by biochemical tests.
Non-Specific Urethritis : It manifests like gonorrhoca with burning sensation in the urethra during micturition with the differen that the urethral discharge/vaginal discharge is mucoid rather than purulent and the gonococcus can not be demonstrated by smear or by culture. Most of these cases are caused by Chlamydia trachomatis while a major proportion of the remaining cases are attributable to Ureaplasma urealyticum(mycoplasma). Similar symptoms may sometimes be caused by Candida and Trichomonas vaginalis and less commonly other organisms.
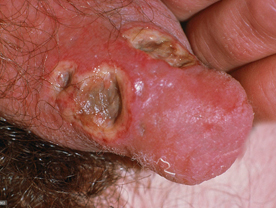
Chancroid : It is caused by a Gram negative rod-shaped organism called Haemophilus ducreyi. The incubation period is 1-5 day and the characteristic lesion consists of a superficial well defined ulcer which has reddish granulation on the floor it is painful on touch and bleeds on manipulation. The ulcers are usually multiple. Within a few days the regional lymph node (usually in the inguinal region) becomes enlarged and tender and becomes soft to form a unilocular swelling and ruptures. Even if the disease is not treated the ulcer tends to heal. The infection does not become chronic or disseminates to other parts of the body. The diagnosis is usually made on the basis of clinical
criteria. But in about 30-50% of the patients it may be possible to demonstrate the presence of the organism in the smear prepared from the discharge from the ulcer or pus from the lymph node and stained with Gram's stain.
Gram negative organisms lying in chains or a school of fish formation are characteristic. Culture of the organism on artificial media is also often unsuccessful.
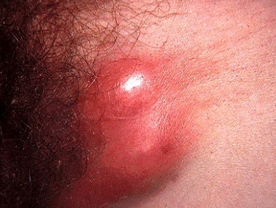
Lymphogranuloma venereum : It is caused by a virus like agent Chlamydia trachomatis The first lesion is a small herpetiform vesicle or an ulcer which appears 3-5 weeks after the infection but the lesion is so small and evanescent that it is usually missed by the patient. The first manifestation therefore generally noticed by the patient consists of enlarged and tender lymph nodes which soon become matted and rupture to form multiple sinuses discharging thin purulent material. Involvement of the lymph nodes above the inguinal ligament along with the involvement of the lymph nodes below the inguinal ligament produces the groove sign characteristic of LGV Some patients may also develop fever, chills, nausea and even loss of appetite. The diagnosis is usually made on the basis of clinical criteria
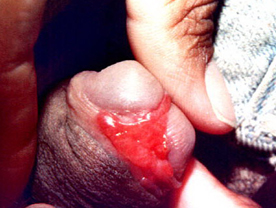
Donovanosis : It is also called granuloma inguinale and is caused by Donovania graulomatis. The incubation period is 7-30 days but it may extend to even several years. The infectivity of the organism is very low. The lesion consists of an irregular ulcer which looks fleshy and bleeds on touch. A lesion in the inguinal region may be mistakenas an enlarged lymph node and is therefore called pseudo-bubo. The lesion is slowly progressive and it may last several years.
The diagnosis can be confirmed by preparing a smear from the granulation tissue, staining it with Giemsa stain and demonstrating the organism inside the macrophages The organism produces a safety-pin like appearance which is very characteristic

